What Causes a Ruptured Disc to Develop?
A ruptured disc is, in essence, a form of disc herniation. For a broader explanation of disc symptoms, movement changes, and non-surgical care options, visit our herniated disc care page.
A ruptured disc usually develops gradually rather than suddenly. In many cases, the outer disc layer weakens over time due to repeated stress, prolonged sitting, posture habits, lifting mechanics, and age-related disc changes. Once the outer layer can no longer contain the inner disc material, part of the disc may move outward and begin to affect nearby tissues or nerves.
This page focuses specifically on how a ruptured disc develops, why it most commonly affects the neck and lower back, and what factors may increase disc stress over time.
KEY TAKEAWAYS
- A ruptured disc is a type of disc herniation
- Most ruptured discs develop gradually over time
- Sitting, bending, and repeated loading increase disc stress
- The lower back and lower neck are the most common regions
- Nearby nerves may become irritated when disc material moves outward
How a Disc Bulge Can Progress Toward a Ruptured Disc
Disc changes often develop in stages rather than all at once. This short video explains how a healthy disc may progress from early bulging to herniation and eventually to a ruptured or extruded stage.
Key Moments in This Video
00:00 — Introduction to disc bulge, herniation, and spine-related neck & back symptoms
00:23 — How common spinal disc and joint changes are
00:35 — The role of spinal discs during movement and loading
00:46 — Understanding the nucleus and annulus disc structure
01:10 — How early disc damage begins over time
01:28 — How the outer disc layer develops a tear
01:45 — Which comes first: bulge or herniation?
02:09 — Disc stages: bulge → herniation → extrusion
02:43 — How disc location may influence arm or leg symptoms
Watching how disc changes progress from bulge to rupture can make it much easier to understand why symptoms and movement changes vary from one person to another.
What You’ll Learn About a Ruptured Disc
How a Ruptured Disc Develops Over Time
In most cases, a ruptured disc does not begin as a sudden event.
It often starts with gradual structural changes.
Over time, the disc may lose hydration and become less resilient.
This may happen with:
- prolonged sitting
- repetitive forward bending
- poor lifting mechanics
- repetitive twisting under load
- long hours of driving
- reduced movement variety
As these stresses continue, the outer disc fibers may begin to weaken.
Once the outer layer develops a tear or weakened region, the inner material may move outward.
This is when the disc is commonly described as ruptured.
Why the Lower Back and Neck Are Common Sites
Ruptured discs most often affect areas of the spine that handle the greatest mechanical stress.
In the lower back, the most common levels are:
These levels absorb significant pressure during:
- sitting
- lifting
- transitions from sitting to standing
- bending
- carrying body weight
In the neck, common levels include:
These segments experience repeated loading from head posture and forward neck positioning.
How Posture and Sitting Increase Disc Stress
Long periods of sitting and sustained sitting may increase and poor posture may increase pressure inside spinal discs, especially in the lower back and lower neck.
This is more common when sitting involves:
- slouched posture
- forward head position
- unsupported lower back
- prolonged desk work
- long-distance driving
Over time, repeated compression may affect how the disc distributes load and maintains hydration.
Sitting alone does not directly cause a rupture. Instead, it becomes one of several factors that may gradually increase stress on the disc over time.
This is why movement breaks, posture awareness, and regular position changes are often important parts of spinal care planning.
How a Ruptured Disc May Affect Nearby Nerves
When disc material moves beyond its usual boundary, nearby nerves may become irritated.
This may occur inside the spinal canal or near the opening where the nerve exits the spine.
Depending on the level involved, people may notice changes such as:
- neck discomfort with arm symptoms
- back discomfort with leg symptoms
- tingling
- numbness
- muscle weakness
- changes in walking or balance
The exact symptom pattern often depends on the spinal level and the degree of nerve involvement.
How a Ruptured Disc Differs From Other Disc Changes
Not all disc changes are the same. A disc may progress through several structural stages.
These can include:
- disc bulge
- disc protrusion
- ruptured disc
- disc extrusion
A ruptured disc generally refers to a more advanced stage in which the outer layer no longer fully contains the inner material.
For more advanced structural stages, see our extruded disc page.
Human Spinal Disc
Spinal discs are avascular structures. In other words, they do not have a direct blood supply. Nutrients are diffused inward to comply with the demands of the spinal disc cells. The diffusion of nutrients takes place through the vertebral end-plate. The vertebral end-plates are less than 1 mm thick and embedded in the bones of the spine.
Contrary to common belief, these vertebral end-plates are not part of the vertebra but part of the spinal disc. It serves the spinal disc by providing an anchoring point to the vertebra and a structure through which nutrients must diffuse. Injury and neglect of minor spinal conditions lead to a malfunction to end-pates and an eventual interruption in the flow of nutrients to a spinal disc. Continued disruption in the flow of nutrients is the leading cause of a herniated disc.
Lack Of Blood-Flow Is The Leading Causes Of Disc Degeneration & Eventual Slippage
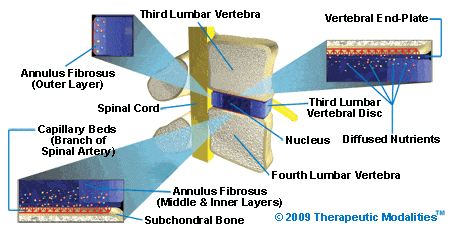
Disc cells manufacture the aggrecan (protein molecule that is the building block of disc cells) molecules. Disc cells continuously create, replace, and rebuild the aggrecan molecules. As long as the disc cells have a proper uninterrupted flow of nutrients (water, glucose, amino acids, and oxygen) and a non-acidic environment, the spinal disc can rebuild and help as needed. An interruption in the flow of nutrient flow for the starving discal cells leads to degenerative changes. These degenerative changes, in turn, lead to a more severe disc condition such as a bulging or herniated disc.
Often, a herniated disc compresses the sensitive nerve fibers as they exit the spine. The compression of these fibers can lead to a local or radiating discomfort of varying intensity. The most disturbing aspect of a herniated disc is not the discomfort caused by the compression but rather the prolonged compression of the spinal cord or nerve.
How Care Is Commonly Structured Without Surgery
Non-surgical care often focuses on how the spine moves, loads, and adapts during daily activity.
This may include:
- gentle chiropractic methods
- physiotherapy
- rehabilitation exercise
- movement retraining
- posture correction strategies
- guided strengthening
The goal is to understand how disc stress developed and how daily mechanics can be improved.
Related Disc Pages
For a full understanding of disc conditions, you may also find these pages helpful:
This strengthens your topical cluster significantly.
Recap — What to Know About a Ruptured Disc
A ruptured disc usually develops gradually rather than all at once.
Repeated loading, prolonged sitting, posture habits, reduced hydration, and weakening of the outer disc fibers may all contribute to how the disc changes over time.
The lower back and lower neck are the most commonly affected regions because they absorb the greatest daily mechanical stress.
Understanding how the rupture develops helps explain why symptoms, movement changes, and nerve-related patterns can vary from person to person.
About the Author of What Causes a Ruptured Disc to Develop?
Author of What Causes a Ruptured Disc to Develop?: “What Causes a Ruptured Disc to Develop?” was written by Yama Zafer, D.C., who has an educational background in chiropractic from Cleveland University–Kansas City and has dedicated nearly three decades to chiropractic, physiotherapy, and rehabilitation care; read more on Y. Zafer.
Last Updated:
Last updated on April 2, 2026: What Causes a Ruptured Disc to Develop?
Frequently Asked Questions About Ruptured Disc Causes and Care
A ruptured disc often develops gradually over time rather than from a single moment. The questions below explain how disc changes progress, what may increase disc stress, how nearby nerves may be affected, and how care is commonly structured without surgery.
What usually causes a ruptured disc to develop?
Can sitting cause a ruptured disc?
Which spinal levels are most commonly affected?
Can a ruptured disc affect nearby nerves?
Is a ruptured disc the same as a herniated disc?
Can a ruptured disc develop gradually?
Can a ruptured disc happen in the neck?
How is care commonly structured without surgery?
Share with others:
